Is the criticism legitimate, and what’s wrong with the evidence?
Aside of all the opposition and criticism of the homeopathic treatment approach, it has to be acknowledged, even by sceptics, that homeopathy seemingly provides numerous advantages over conventional medical treatment. Not only is it a gentle non-invasive approach that employs remedies that are, generally speaking, non-toxic and devoid of harmful adverse effects, but it also boasts a holistic, totality encompassing treatment that aims to strengthen the body´s own natural defences and as such rapidly assists the recovery from illness. Unlike conventional medical drugs, homeopathic remedies do not suppress an active ailment, but aid the body in its self-healing response to the sickness, and at that aim to remove the root cause of the presenting illness.
Yet critics and opposers of the homeopathic treatment approach do not accept these arguments, and even reject the extensive patient reports confirming the efficacy of homeopathic treatment. These Sceptics build their opposition on one major point of critique, namely that of a lacking evidence base. They most commonly criticize that homeopathy has no solid scientific research supporting its claim of efficacy. Yet, the antagonism on this account stands on very wobbly ground.
Is everything as it is claimed?
The conventional medical sphere insists, even demands that therapeutic disciplines, in order to be considered as safe interventions and treatment options, must be supported by thorough research, and hence be accredited as effective according to the existent medical paradigm. With such insistence, logically, the provision of an evidence base should measure up to the same standards for all health care approaches, and in particular for conventional medicine! Yet, how well does orthodox medicine measure up to its very own standards?
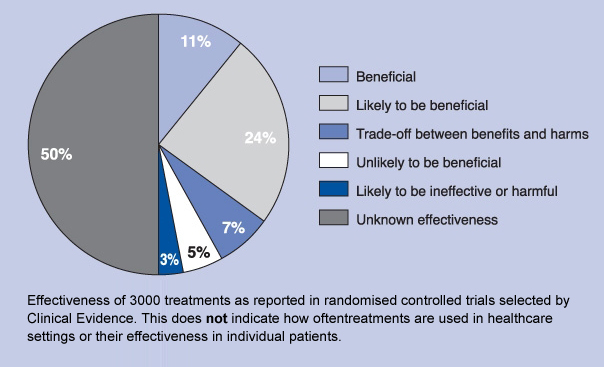
According to an appraisal conducted by ‘Clinical Evidence’, a BMJ (British Medical Journal) database, in which it reviewed the benefits and harms of 3000 conventional medical treatments, orthodox healthcare fared rather feebly [1].
http://clinicalevidence.bmj.com/x/set/static/cms/efficacy-categorisations.html
The appraisal brought to light a rather extensive discrepancy, as a mere 11% of investigated studies provided outcomes that suggested the trialled treatment was one to be of benefit to patients. 24% were found to be likely to be beneficial, and for 7% it was unclear whether the intervention was beneficial or actually harmful. This gives a percentage of 42 of interventions, where some benefit of the treatment is potentially given. Only!
This figure is quite as shocking, because that calculation leaves 58%, more than half of the investigated studies, with outcomes from ‘unlikely to be beneficial’, ‘ineffective or harmful’, to of ‘unknown effectiveness’. This means that 58% of treatments, failed to provide any proof of efficacy, were dangerous, or delivered results that were non-compliant with the classification of effectiveness. As such conventional medicine failed to be compatible with its self-imposed standards of providing evidence of efficacy! It failed to meet those standards that it claims all other health care practices should be measured against, which, in the argumentum e contrario, means that it should itself not be classified as a safe treatment practice.
In this light, the persistent critique of and the antagonism toward the homeopathic treatment approach and CAM in general, appears entirely inept. Conventional medicine stumbles across its own, highly set standards and fails to provide treatments that are found to be consistently effective, while demanding exactly such an evidence base from CAM.
What about the state of evidence of efficacy for homeopathy?
Until the beginning of 2014, 104 placebo-controlled trials had been conducted investigating diverse ailments that had been treated homoepathically [2]. A detailed review of these has delivered similar outcomes as had been reported from the review by Clinical Evidence above. 41% of studies had reported an effectiveness of the homeopathic treatment, 5% showed homeopathy to be ineffective, and 54% of studies had an outcome that was inconclusive.
Yet, these outcomes do not validate the same criticism, as is voiced considering the outcomes of the conventional medical appraisal. For, what must be considered in the comparison of this review of homeopathic trials to the above review of studies of conventional medicine, is the difference in the quantity of trials appraised. For conventional medicine there were 3000 studies, and for homeopathy only 104 that were investigated.
This pronounces a general problem with investigations into homeopathy, and, at that, all of CAM. For the alternative and complementary health practices a much smaller body of evidence is available due to the lack of funding of quality research.
What´s wrong with the research into homeopathy?
The controversy though prevails, and skeptics will continue to criticize the homeopathic treatment approach on the pretense that there simply is nothing in it, and that research has not been able to provide stable evidence of efficacy. In the consequence of research supporting homeopathy, the opposers of this gentle healthcare approach still, consistently deny the same, fail to correctly interpret and actually understand it. Beyond this, they hail all research that disproves or at least questions the efficacy of trials and studies coming to conclusions of effectiveness of homeopathy.
So, what is wrong with the research into homeopathy? Dr. Iris Bell, in a paper published in the Journal of Alternative and Complementary Medicine [3], brings the discrepancies in research to the point. She highlights what is wrong with one of the most frequently cited studies when it comes to demonstrating the so-called absence of efficacy of homeopathy, the Shang et al. meta-analysis [4]. In doing so, she outlines the crux with the prejudiced stance of conventional medicine towards homeopathy.
Besides methodological flaws in the Shang et al. study, Bell points out that as much in this meta-analysis, as in overall research into homeopathy, most fails to acknowledge the homeopathic philosophy underlying the treatment approach. She criticizes meta-analyses that include studies trialing similar approaches that are often mistakenly labeled as homeopathic, albeit following different principles. She mentions ‘isopathy’ as one such example. Furthermore, Bell stresses that homeopathic prescriptions under investigation, are mostly selected on the grounds of an allopathic diagnosis; following the principle of ‘one fits all’. This is of course totally contrary to the concept of individualization advocated by Hahnemann, and fundamental to the homeopathic treatment approach. The remedy given therefore, is for numerous patients, inappropriately prescribed, narrowing positive treatment response from the very start.
Bell emphasizes that homeopathic medicine trialed by a conventional framework cannot yield outcomes true to the treatment approach. She stresses that a study design is needed that is sensitive to homeopathic principles and its practice, and as such, does justice to aspects other than the conventional medical trial parameters.
She furthermore advises that trial investigations are intended to reflect outcomes as closely as possible met in real-life scenarios. Yet, the conventional research investigation only partially meets this criterion. Homeopathy in application for patient health care, is therefore a much greater reflection of efficacy than can ever be extrapolated from research conducted in the conventional framework.
While the demand for evidence based medicine practice is certainly warranted, and interventions and treatments need to be monitored for their applicability in practice, evidence of efficacy derived from clinical practice cannot be ignored. This is as much true for holistic treatment approaches, like homeopathy, as it is for conventional medicine. While conventional medicine leads and dictates the sphere of scientific research, homeopathy is particularly strong when it comes to its experiential clinical practice.
Is the rejection of homeopathy, and CAM in general, a valid approach?
Taking into consideration this evidence of CAM delivered from the experiences in practice, and what this tells us about patients and their needs, it becomes evident that aside of the debate over the efficacy supported by an extensive research base, the need for CAM practices cannot be dismissed or rejected.
CAM practices deliver aspects of care that have long been abandoned in conventional medicine, where the lack of time in the consultation, the workload of doctors, the adverse effects of conventional medication and interventions, provide little space for aspects of the therapeutic environment that come from being there, listening, understanding and supporting, aside of the machinery and pills prescribed. Yet, these aspects can be influential on general well-being, compliance and treatment effect.
Furthermore, even if we follow up on the argument that CAM treatments are solely due to placebo, their validity still stands strong as studies have shown that placebo is able to instigate significant biological effects that frequently can be of similar impact to those achieved by medication [5].
Is the criticism legitimate, and what’s wrong with the evidence?
Despite the failings of allopathy in providing the irrevocable evidence of effectiveness in its own scientific research, it is viewed as ‘evidence based’ medicine, and does not cease to denunciate CAM practices for their apparent lack of the same. It would suit orthodoxy well, to refrain from its persistent critique in the light of such appraisals as that conducted by ‘Clinical Evidence’. Both, mainstream medicine and CAM could benefit of research methodologies that are sensitive to holistic implications of, and on a health care regimen or treatment intervention.
Patients are individuals, and their totality, habits, preferences, etc. in terms of their health care and their normal life-style, are influential on treatment outcomes. The eventual effectiveness of an intervention, in practice, is therefore equally if not of superior importance to its scientific evidence according to a predisposed framework. In terms of the former, conventional medicine is struggling, and with the latter, not exactly faring well. Perhaps mainstream medicine should look more at what it can learn from the CAM therapies rather than try to criticize and vilify them without having appropriately investigated and appraised them.
Reference:
[1] BMJ (2012) ‘What conclusions has Clinical Evidence drawn about what works, what doesn´t based on randomised controlled trial evidence? ‘, Clinical Evidence, [Online]. Available at: http://clinicalevidence.bmj.com/x/set/static/cms/efficacy-categorisations.html (Accessed: November 2015).
[2] Homeopathy Research Institute (n.d.) “There is no scientific evidence that homeopathy works”, Available at: https://www.hri-research.org/resources/homeopathy-the-debate/there-is-no-scientific-evidence-homeopathy-works/ (Accessed: November 2015).
[3] Bell, I. (2005) ‘All Evidence Is Equal, but Some Evidence Is More Equal than Others: Can Logic Prevail over Emotion in the Homeopathy Debate?’, The Journal of Alternative and Complementary Medicine, 11(5), pp. 1-20 [Online]. Available at: http://www.researchgate.net (Accessed: 31 October 2015).
[4] Shang A, Huwiler-Müntener K, Nartey L, Jüni P, Dörig S, Sterne JA, Pewsner D, Egger M. (2005) ‘Are the clinical effects of homoeopathy placebo effects? Comparative study of placebo-controlled trials of homoeopathy and allopathy.’, Lancet, 366(9487), pp. 726-32 [Online]. Available at: http://www.thelancet.com (Accessed: 31 October 2015).
[5] Marchant, J. (2015) ‘Consider all the evidence on alternative therapies’, Nature, 526(), pp. [Online]. Available at: http://www.nature.com/news/consider-all-the-evidence-on-alternative-therapies-1.18547 (Accessed: October 2015).



Quality of Trials in Homeopathy superior to conmed (19% vs 8%) (Shang et.al., Lancet 2005)
Posted by Dr. Nancy Malik | 12/12/2015, 4:55 PM